Post-Acute Care and Interoperability
| 3.13.19 By Erik Bermudez, KLAS |
With the recent announcement about the CommonWell-Carequality connection, interoperability is a hot topic in the healthcare world. But at KLAS’ Digital Health Investment Symposium (DHIS) in August, I got to discuss the state and importance of interoperability in one critical piece of the healthcare continuum: post-actue care.
DHIS 2018 hosted some of the industry’s greatest minds on topics from revenue cycle to precision medicine. Our post-acute panel discussion boasted two experts: Bob Latz, CIO of Trinity Rehabilitation Services, and Laurie Neander, President of Bassett Health Network: At Home Care.
As the facilitator of the panel discussion, I got to introduce the topic, our speakers, and some of the intriguing data KLAS has gathered from our provider friends about the state and importance of interoperability in the post-acute world.
Understanding the Gap
I began our conversation by sharing with the attendees two events that helped solidify my passion for post-acute care and my understanding of interoperability in the space.
The first event took place at KLAS’ second Interoperability Summit in 2016. Thought leaders from provider and vendor organizations gathered to discuss how we could address issues with interoperability. At end of the session, we asked the attendees, “How can we make our next summit better?”
At that point, one attendee stood up and said, “You’re missing a key voice in the spectrum of healthcare, and that is the post-acute side. They are a huge part of the puzzle when it comes to solving interoperability.”
This comment hit home. Ultimately, it led KLAS to pick the brains of providers and create a survey to measure the status of interoperability in the post-acute space. I’ll discuss parts of the resulting report later.
The second event took place during this same period. I was speaking with a friend who was a director of admissions and intake. When we got to the topic of interoperability in the post-acute space, he said it was nonexistent.
“When I know I am going to receive a patient,” he said, “it’s faster for me to drive to the hospital and pick up a patient’s record than to wait around for a fax that would take hours to come through and be incomplete anyway.”
Understanding the significant gaps post-acute stakeholders face, particularly in terms of interoperability, made me want to get involved. Luckily, my wish was granted. I got to work on and coauthor our Post-Acute Care 2018 report, which sports the subtitle, “Providers’ Simple Request: ‘Help Me Connect’”.
Insights from the Post-Acute Care 2018 Report
We took a few minutes at DHIS to review some findings from the report. We first discussed with the attendees the question of how post-acute providers are most likely to access outside data. Unfortunately, faxing was the top response.
As many would guess, acute care providers are accessing much more outside data electronically than post-acute providers are. We showed DHIS attendees the following chart to illustrate the disparity.

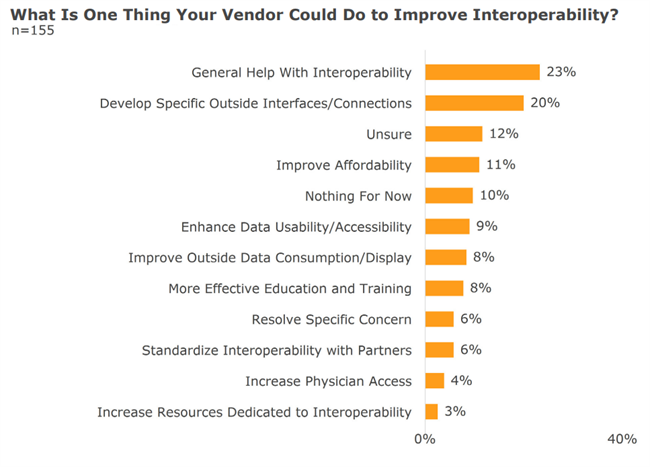
Clearly, vendors have been focusing less on interoperability in the post-acute space than is needed. To that tune, our survey had also asked post-acute providers this question: “What is one thing the vendor could do to help drive interop success?”
The most common answer, “General Help With Interoperability”, mainly encompassed awareness and simple hand-holding. Help with specific interfaces was second on the list. The fact that the top two answers were arguably the most basic ones is more evidence that post-acute vendors need to invest much more in their interoperability efforts.
The Key to Transitions of Care and Value-Based Care
Almost everything discussed at our post-acute panel related to interoperability, even if the connection wasn’t immediately obvious. For example, when we opened the panel up for questions, one audience member asked, “What about the transitions of care between acute care, skilled nursing, and home health? How are those transitions working?”
Panelist Laurie Neander was quick to respond. “Those areas are still fairly siloed for us,” she said. “The lack of interoperability is still a big issue. We have access to data in a secure database, but we have to dig through too much data to find what we are looking for. In some cases, we’re even told by Medicare that the data we send them isn’t enough.”
“We could do so much by focusing on transitions of care,” Bob Latz said, also noting the importance of interoperability. “The different areas have to be able to talk to each other.”
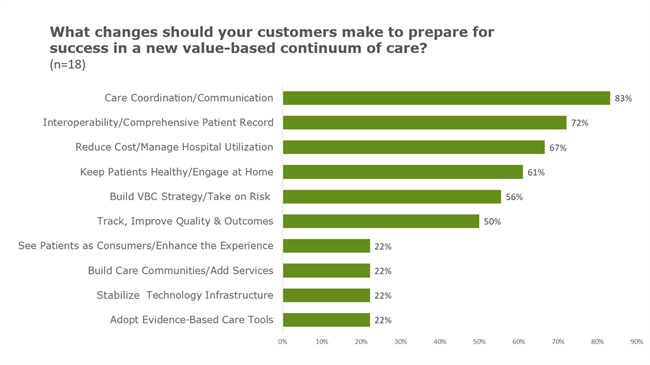
Interoperability also appeared organically in some insights from L.E.K., one of KLAS’ partners sponsoring DHIS. They had asked a number of vendors, “What can your customers do today to become more prepared for the switch to value-based care?”
As you can see from the following chart, which we shared at the DHIS panel, the number-two response was “Interoperability/Comprehensive Patient Record”. Funnily enough, the transitions of care we talked about at the panel could fit under the top answer from L.E.K.’s poll: Care Coordination/Communication.
Apparently, solving every other problem faced by post-acute providers will first require solving the interoperability problem. Nothing gets done without data.
New Energy
Post-acute care is a crucial point on the spectrum of healthcare, and it’s only getting more important over time. As the average age of Americans rises, the demand for home health providers is skyrocketing.
-
More AEHIA News Volume 3, No. 1:
- There and Back Again, A Healthcare IT Journey – Candace Stuart, CHIME Communications Director
- Karen Wilding Reflects on Bootcamp Experience – Ashley Jester, CHIME Professional Development & Membership Specialist
- A Brief Debrief – Zach Donisch, Director, AEHIA Membership
Looking to contribute to the AEHIApplications Newsletter? Email your contributions to [email protected].
